The Trans-NCI Obesity and Cancer Work Group was established in 2019. The purpose of the work group is to promote the exchange of information and cross-cutting interests in obesity and cancer research within NCI. Our activities include the development of meetings, workshops and webinars for staff and public knowledge, and the development of scientific manuscripts. The work group also conducts portfolio reviews and identifies and promotes new opportunities in obesity and cancer research. Six subgroups have been formed: Prevention, Etiology, and Mechanisms, Treatment and Survivorship, Measurement and Methods, Health Drivers, Time-Restricted Eating, and Pediatrics and Physical Activity.
Objectives
- Identify and summarize the state-of-the-science to document what is known and what is needed to move the science forward
- Identify and prioritize critical research questions/needs/gaps in each topic area
- Develop research concept themes and other activities to stimulate research
- Plan and develop a webinar series with topics related to the different subgroups
Featured Obesity and Cancer Initiatives
Subgroups
The Prevention, Etiology, and Mechanisms subgroup is exploring the following challenges in obesity and cancer:
- What are the risk factors, biological mechanisms and pathways associated with obesity/overweight and cancer as it relates to excess body weight and/or adiposity driving the development of pre- and invasive cancers across the lifespan in all populations across geographic locations?
- Does overweight/obesity in children and youth increase the risks for cancer development later in life?
- How do risk factors, such as sleep, stress, social determinants of health, the microbiome, metabolic and immune dysfunction, environmental obesogens, influence and/or interact with mechanisms through which obesity might increase risk of cancer?
- What effective strategies could prevent or intercept mechanistic biological changes such as inflammation, immune function, and metabolic dysregulation of obesity associated cancers?
- Does the timing, duration, and amount of weight loss in the life cycle influence cancer risk (i.e. in childhood/youth versus adult)?
- Which interventions decrease obesity and associated unhealthy lifestyle behaviors, applied across the lifespan, to reduce and/or delay cancer incidence?
The aims of this subgroup are related to the Metabolic Dysregulation and Cancer Risk Program, a transdisciplinary NCI initiative to enhance knowledge of the dynamics and underlying mechanisms that link obesity, metabolic dysregulation, and increased cancer risk.
Co-Chairs
Linda Nebeling [DCCPS]
Ed Sauter [DCP]
Wanping Xu [DCB]
The Treatment and Survivorship subgroup is exploring the following challenges in obesity and cancer:
What are the effects of diet, exercise and body composition on cancer treatment efficacy & outcomes?*
- Need better characterization of optimal type, dose, frequency, duration, timing of exercise and diet as well as nutritional status on chemotherapy uptake, adherence, side effects, treatment response & clinical outcomes as it relates to obesity and cancer.
- Explore the relationships between obesity/body composition, cancer progression, and response to treatment.
- Study how diet, exercise, body composition, and nutritional status impact cancer-related symptoms and quality of life.
What are the effects of obesity/body composition, exercise & dietary regimens on post-treatment outcomes?*
- Need better characterization of post-treatment exercise and diet interventions on long-term treatment related toxicities and clinical outcomes, QoL, sleep, and general health outcomes.
- Explore how nutritional status and changes in nutritional status affect post-treatment outcomes.
- Need to understand how weight maintenance/loss interventions during treatment affect outcomes and survival.
- Need better precision weight maintenance/loss interventions for post-treatment cancer survivors.
*These questions need to be addressed across cancer sites/subtypes, stage of diseases, and in various groups of survivors with respect to age, body size, activity level, and more.
Co-Chairs
Tanya Agurs-Collins [DCCPS]
The Measurement and Methods subgroup is exploring the following challenges related to obesity and cancer:
- How can complementary assessment methods (e.g., self-report, sensor-based technologies, and/or biomarkers) be triangulated to improve insights into diet, physical activity, and sleep behaviors and environmental determinants?
- What assessment and analytic methods are needed to better integrate measures of diet, physical activity, and sleep within the 24-hour day?
- How can assessment tools for modifiable risk factors be developed or adapted and validated for cancer survivors?
- How can methods be enhanced to measure the food and physical activity environment in various populations using appropriate reference instruments?
Co-Chairs
Jill Reedy [DCCPS]
Dana Wolff-Hughes [DCCPS]
The Health Drivers subgroup is exploring the following challenges in obesity and cancer:
Why do cancer and the health consequences of obesity disproportionately affect some populations more than others?
- Geography, economy, genetic and epigenetic predisposition, occupational and environmental health exposures, health care access, internet access, communication, differences in lifestyle, and more all contribute to the impact of the ability of patient populations to seek and receive cancer information and care related to cancer prevention, screening and treatment - including risks/benefits associated with various treatment modalities.
- Need for greater understanding of the intersection and interplay among upstream and downstream determinants of health on cancer.
- Enhance understanding of the underlying protective and risk factors associated with rising obesity rates.
How can we tailor interventions influencing weight loss, exercise & dietary regimens to have better outcomes in different populations to reduce cancer risk?
- Better characterization of optimal prevention strategies and delivery of interventions, type, dose, frequency, duration, timing of exercise & diet on health behavior outcomes & QoL.
- Identify evidence-based interventions and preventative strategies to improve weight, physical exercise, and diet, including effective ways to address barriers, such as those relating to SES and environmental constraints (e.g. time constraints) that pose obstacles to implementing such strategies.
Co-Chairs
Tanya Agurs-Collins [DCCPS]
Anil Wali [CRCHD]
The Time-Restricted Eating subgroup is exploring the following challenges in obesity and cancer:
- What are the effects of time-restricted eating (TRE) compared to other diet strategies, including, but not limited to, caloric restriction or other intermittent fasting approaches, on weight loss, weight maintenance, and long-term dietary adherence?
- What role does TRE play in reducing cancer incidence and progression, cancer treatment response, and cancer recurrence?
- What are the emerging obesity risk factors, including the hormonal milieu, microbiome, and epigenetic modifications that impact TRE’s efficacy?
The TRE subgroup is following NIH/NCI supported projects and their impact on cancer endpoints, including:
- A project that evaluates the impact of TRE on cancer cell growth for breast cancer between diagnosis and definitive surgery
- Two projects, one in lean and the second in overweight/obese individuals, on cancer risk endpoints
- Four TRE projects evaluating the impact of TRE on risk of breast and colorectal cancer
Co-Chairs
Ed Sauter [DCP]
Tanya Agurs-Collins [DCCPS]
The Pediatrics and Physical Activity subgroup is exploring the following challenges in obesity and cancer:
- What is needed to accelerate the application of pediatric exercise and physical activity intervention knowledge from bench to bedside to communities beyond?
- What are research opportunities for exercise, physical activity and physical education for pediatric cancer patients and survivors?
- What role do pediatric exercise and physical activity interventions play in improving cancer treatment outcomes?
Co-Chairs
Heather Bowles [DCP]
Frank Perna [DCCPS]
Obesity & Cancer Webinar Series

The Obesity and Cancer Webinar Series includes a wide range of obesity and cancer topics. Past webinars have focused on the following topics as related to cancer and obesity: time restricted eating, sleep and circadian rhythm, COVID-19, health disparities, inflammation and insulin resistance, microbiome, and physical activity interventions.
Recordings of these webinars, and information on planned webinars, is available at the following link:
Additional Information
- Dietary Assessment Resources
- Exercise and Nutrition Interventions to Improve Cancer Treatment-related Outcomes (ENICTO) in Cancer Survivors
- Metabolic Dysregulation and Cancer Risk Program: A Transdisciplinary Approach to Obesity-Associated Cancer Research
- National Collaborative on Childhood Obesity Research. Advancing Measurement for Childhood Obesity Workshop Series
- NIH Obesity Research Task Force
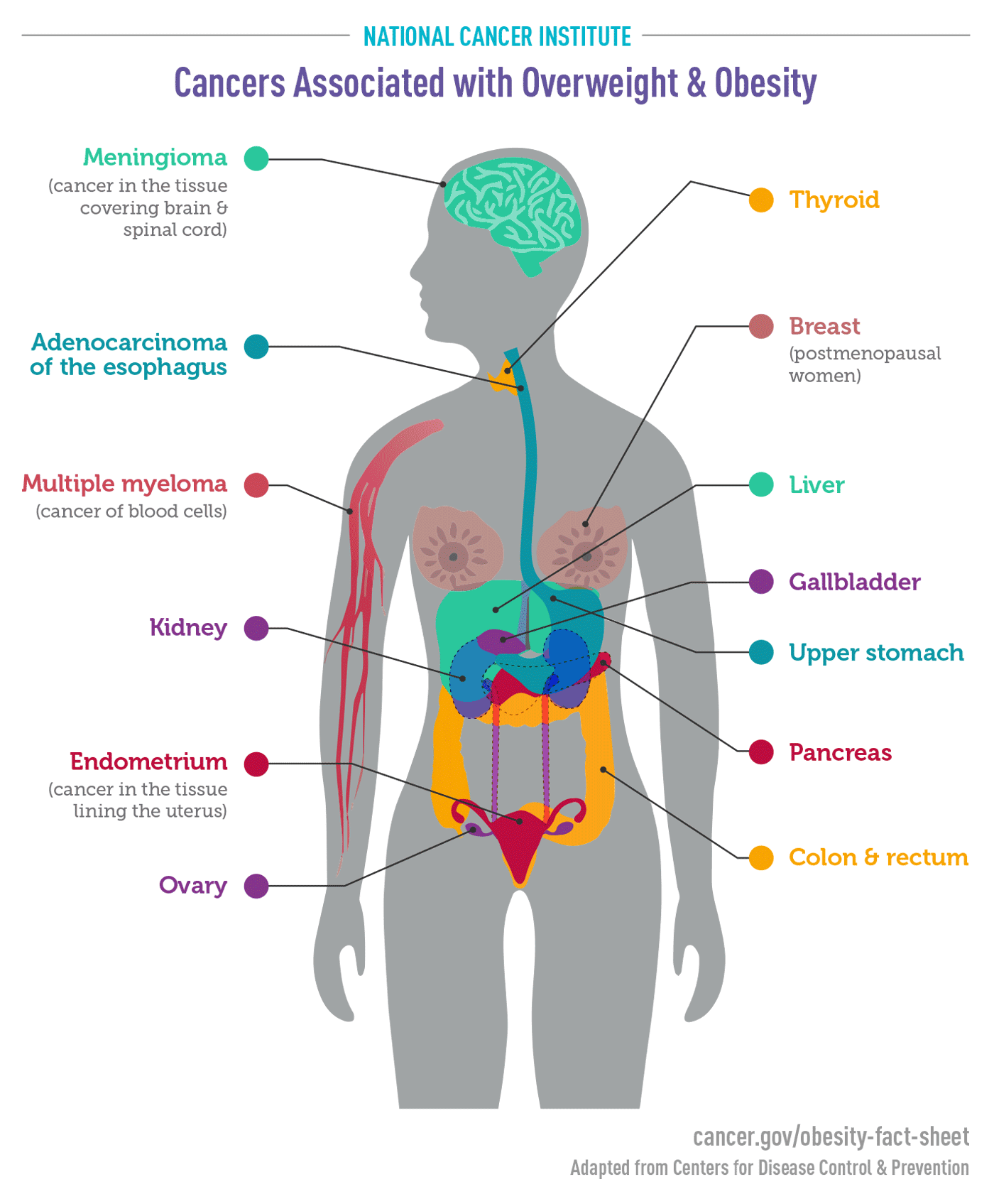
- Obesity and Cancer Fact Sheet, NCI
- Physical Activity Assessment Resources
Contacts