1. Description and Theoretical Background
Definition
The concept of perceived barriers has been used in behavioral medicine for a long time in one form or another. The earliest widespread use of the barriers concept was associated with the Health Belief Model, as described in the following section. Webster's dictionary defines a barrier as "something that impedes or separates". Interestingly, the concept of barriers to accomplishment of a goal or a specified health behavior is assumed to be so straightforward that it is often left undefined. For the purposes of this summary, perceived barrier will be defined as "a person's estimation of the level of challenge of social, personal, environmental, and economic obstacles to a specified behavior or their desired goal status on that behavior."
This definition raises a number of issues. First, the adjective "perceived" (barriers) implies that the individual's judgment about the number and strength of barriers is a cognitive process; as such, this judgment may or may not be closely aligned with "objective" measures of social, environmental, or economic barriers. Many factors in addition to "objective barriers" influence a person's perception of barriers. Several of these factors, including past history, risk or threat perceptions, and perceived social support, influence beliefs about barriers. Figure 1 summarizes the presumed interactions among perceived barriers, "objective barriers," other psychosocial factors, facilitators or promoters, and potential background moderating variables. This figure is an attempt to synthesize the literature and to represent commonalities across theories and several of the key research issues—it is not based on any one theory.
Self-Management, Adherence, and Compliance
We assume that perceived barriers (and other factors) in turn lead to, at minimum, changes in self-efficacy expectations and problem-solving attempts. Self-efficacy and problem solving, along with potential moderating variables, in turn then lead to actual levels of the specified self-management or "adherence" health behaviors. The term self-management is preferred over adherence or compliance to reflect the role of agency and self-determination involved in health-promoting or disease management behaviors (Bandura, 1997; Williams et al., 1998), rather than the more health care provider-centric term of compliance. Finally, the performance of the specified health behavior has consequences. The individual judges her performance and its results, and this judgment in turn reciprocally influences or adjusts one's perception of barriers. Thus, as summarized in Figure 1, perceived barriers are assumed to be malleable based on experience; different for different health behaviors; and influenced by, and in turn, influencing multiple factors.
Figure 1. Logic Model of Role Of Perceived Barriers and Related Constructs to Patient Self Management/Adherence
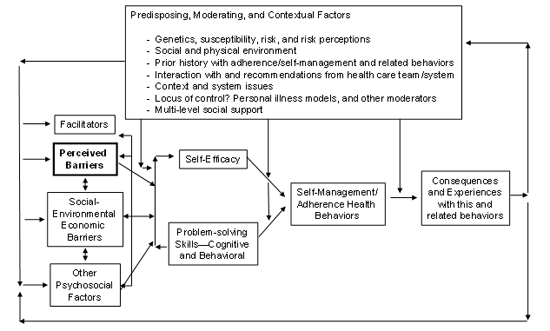
Similar Constructs
Perceived barriers to self-management behaviors should be distinguished from related constructs, such as other health beliefs, self-efficacy expectations, behavioral intentions, personal illness models, and "objective barriers." Figure 1 illustrates the conceptual relationships among several of these constructs. The primary distinguishing feature of a perceived barrier is that it is a judgment of the degree of difficulty of a set of diverse factors (barriers) that can interfere with accomplishment of a specified health behavior. Several factors, such as past experience and one's personal illness model (Hampson, 1996) or illness representations (Leventhal et al., 1991), influence these judgments. Perceived barriers are strongly related to "objective" measurements of barriers, but are not the same. For example, a man facing his first colonoscopy might overestimate the barrier of pain or discomfort he is likely to experience, and this judgment might cause him to delay scheduling the test. Perceived environmental barriers to healthy eating and objective measures of factors such as the number of health food stores and healthy eating establishments in one's neighborhood and work vicinity will usually be related—but imperfectly. As discussed below under measurement issues, there are challenges in separating one's judgment of the magnitude of barriers to a behavior from the judged difficulty of the behavior; and in practice, making this distinction may be impractical. Some investigators have merged the operational measures of barriers and self-efficacy (Glasgow et al., 2001; McCauley et al., 1998) so that respondents are asked to state their confidence that they can successfully cope with specified barriers (barriers-based self-efficacy). This conjunction provides one solution to measurement challenges described below.
Perceived barriers are conceptually distinct from, but related to the concept of perceived power from the theory of planned behavior (McCauley et al., 1998; Montano & Kasprzyk, 2002). Perceived power, defined as the perceived effect of each condition in making behavioral performance difficult or easy, is one of the determinants of perceived behavioral control in this model (Montano & Kasprzyk, 2002). The barriers concept has also been extended to related issues beyond the scope of this report, to include issues such as barriers to strategy adoption, professionals’ barriers to implementation of evidence-based guidelines, organizational barriers to health care system change, barriers experienced by caregivers, and congruence between patient and provider perceptions of barriers (Ruelaz et al., 2007). Finally, the converse issue of facilitators or supports for a given behavior is also an important and, unfortunately, an often neglected determinant of health behaviors (Glasgow et al., 2005). Facilitators and barriers are not just mirror images; conceivably a person could have many or few barriers and many or few facilitators or supports.
2. Use in Health Behavior Theories
Barriers are a central part of many theories of health behavior. The health belief model (HBM) was one of the earliest to prominently feature perceived barriers (Becker et al., 1979) In the HBM, both barriers to and perceived benefits of a behavior lead to the likelihood of taking recommended action (as do other components such as perceived threat).
Perceived barriers are also involved in social cognitive theory (as partial determinants of self-efficacy as illustrated in Figure 1) and social-ecological theory (judgments of barriers are commonly used as proxies for objective measures of multilevel determinants of behavior). Social-ecological theory (Glanz et al., 2002; Stokols, 2000) conceptualizes barriers along a continuum from proximal (e.g., family) to intermediate (e.g., health care team, work-related) to more distal (e.g., community access, media advertising) factors. Perceived barriers are also an important, though largely implicit aspect of goal, goal attainment, and self-regulation theories (Locke et al., 2002; Leventhal et al., 1991). In these theories, goals are established and health behaviors are executed in attempts to attain these goals. Barriers, and how barriers are perceived, interpreted, and addressed, have a large influence on both goal setting and goal attainment. The Transtheoretical Model (TTM) also incorporates the concept of barriers. In the TTM, barriers are called "temptations" and questions framed as "how tempted are you in different situations?" (see Table 2).
Much recent attention has been devoted to social problem-solving theory (D’Zurilla, 1996) and related self-management conceptual models such as the 5 A's: Assess-Advise-Agree upon goals-Assist with problem solving; and Arrange follow-up support (Glasgow et al., 2006; Whitlock et al., 2002). These theories involve identification of specific barriers to self-management, followed by construction and implementation of barrier-related coping or problem-solving strategies (Hill-Briggs, 2003; D’Zurilla, 1996; Glasgow et al., 2007).
The top section of Table 1 summarizes how different theories have explicitly defined perceived barriers and conceptualized barriers. The commonality across these definitions seems to be emphasis on perceptions of the difficulty or psychological costs of different situations-thus, the first part of the definition used in this chapter of "a person's estimation of the level of challenge of social, personal, environmental, and economic obstacles to a specified behavior". The bottom section of Table 1 provides definitions of related concepts, such as temptations or barriers-based self-efficacy that have focused on the impact of barriers on one's confidence or perceived ability. This estimated impact of a barrier is captured in the later part of the definition used in this summary of "estimation of the level of challenge…(to) their desired goal status on that behavior".
Table 1. Definitions Used by Different Theories of Barriers, Related Constructs, or the Impact of Barriers on Key Theoretical Constructs
| Theory | Definition |
|---|---|
| I. Theories Explicitly Defining Barriers or Related Constructs | |
| A. Health Belief Model | One's opinion of the tangible and psychological costs of advised action |
| B. Precaution Adoption Theory | Important issue is "beliefs about difficulty" (of barriers) |
| C. Perceived Power Construct in Theory of Planned Behavior | Perceived effect of each condition in making behavioral performance difficult or easy |
| II. Theories Focused on Impact of Barriers on Key Constructs | |
| A. Barriers-based Self-efficacy in Social Cognitive Theory | Person's confidence…in overcoming barriers to that behavior |
| B. Temptations in Transtheoretical Model | Temptation to engage in unhealthy behavior(s) across different challenging situations |
| C. Secondary Appraisal in Transactional Model of Stress and Coping | Perception of one's ability to change the situation or cope effectively (with situation) |
3. Measures and Measurement
Assessment Procedures
A variety of barrier assessment procedures have been developed for a spectrum of diverse cancer screening behaviors, other conditions including diabetes, HIV, pain, and panic attacks, and specific behaviors including medication adherence, healthy eating, physical activity, smoking cessation, and weight management. A PubMed search for "barriers to adherence" produced 1,002 articles and a search for "barriers to cancer screening" produced 1,346. Various procedures have been used to assess barriers including qualitative interviews, open-ended questionnaires, and structured surveys. Barrier items are sometimes based on theory, sometimes on experience, and occasionally on frequency or strength of endorsement in prior research. Several research programs have developed and revised barrier lists over time as a result of data obtained in prior studies. For example, Champion et al. (2007) have evolved a measure of barriers to mammography over time, as have McCauley and colleagues (1998) for physical activity, and Glasgow et al. (2001) for diabetes self-management. Ideally, barrier items would be culturally appropriate, based on both theory and prior research, and pilot tested with one's target population.
Responses to barrier items have been assessed using scales of frequency, probability, strength of barrier, level of concern, how often the barrier has prevented the desired behavior, and finally self-efficacy level. A few studies have investigated use of a combination of frequency and strength responses, but this strategy has not enhanced predictive validity compared to that of a frequency scale alone (Glasgow et al., 2001).
Validity
A number of analysis procedures have been used to validate barriers measures, but the typical analysis relies on cross-sectional correlations (Glasgow et al., 2001). To justify use as a practical method of predicting future behavior, a better strategy would be to determine that a barrier instrument explains incremental variance over and above that explained by simple and more easily obtained variables, such as demographics and past behavior. (For explanatory purposes and to understand why, for example, demographic subgroups may have different levels of cancer screening, a barrier instrument may still be useful). In addition, stronger conclusions can be made based upon prospective than cross-sectional analyses of predictive validity. The issue of how respondents make judgments about barriers is of particular concern. Especially problematic are scales and analyses that a) ask the respondent to rate how often a given barrier caused the person to not be able to engage in behavior X (see Glasgow et al., 2001, for more details), and then b) use this rating to predict concurrent self-reports of behavior X. For example, part of my judgment of "how often the weather prevented me from exercising" is based upon my frequency of exercise. It then does not make sense to use such a barrier measure to predict exercise frequency, since the self-assessment of exercise frequency is part of both barrier and exercise constructs.
4. Common Barriers
There are both similarities and some differences across health behaviors in the types of barriers endorsed most frequently or perceived as most problematic. For example, there is reasonable congruence between the types of barriers endorsed most often for mammography and Pap smear screening: misinformation, embarrassment/discomfort, and inconvenience (Glasgow et al., 2000; Champion et al., 2007). For lifestyle behaviors such as healthy eating, exercising regularly, and smoking cessation, key barriers appear to be social-environmental-peer pressure, negative emotions or mood, stress, and habitual patterns associated with undesired behaviors (Glasgow et al., 2001; McCauley et al., 1998; Velicer et al., 1990). Similarly, commonly endorsed barriers to medication adherence include cost, side effects, and forgetting (Chao et al., 2005).
5. Barriers Related to Cancer: Measurement and Methodological Issues
Given the limited scope of this review, I have focused on 1) barriers to cancer screening, 2) barriers to health behaviors related to cancer prevention and management-such as cigarette smoking cessation, exercise, and following a healthy eating pattern, and 3) a scale that uses response options not covered above.
Characteristics of some of the most widely used barriers to self-management scales are summarized in Table 2. As can be seen, there is variability across almost all of the scale characteristics in Table 2 including target behavior, response type and scale, reliability and validity data, as well as primary purpose of the barrier instruments. Three scales in Table 2 assess barriers to different types of cancer screening. These scales have been developed primarily to help tailor psychosocial interventions (Champion et al., 2007; Glasgow et al., 2000). As can be seen, such papers tend to report fewer data on traditional psychometric characteristics, since the focus tends to be on individual barriers used to tailor individualized recommendations (Zheng et al., 2006). Many investigators conceptualize barriers as a multi-dimensional construct and would not predict that a person's perception of one barrier should strongly predict their perception of other barriers. From this perspective, psychometric measures of internal consistency are less appropriate than other criteria, such as predictive validity and usefulness for tailoring intervention. The other primary use of barrier scales has been to predict health behaviors/adherence. Typically, average or total barrier responses across items are most often used for such purposes (see Appendices 1 and 3).
Table 2. Characteristics of Barriers to Self-Management Scales
| Measure | Target Behavior | Response Scale | Reliability | Validity | |
|---|---|---|---|---|---|
| Test-Retest | Internal Consistency | ||||
| Barriers temptations (Velicer et al., 1990) - Appendix 1 | Smoking Cessation | 1-5 "how tempted" | Not reported | ∝ = .80 - .95 | Three factors or components to structure of temptations scale |
| Mammography barriers - Appendix 2 (Champion et al., 2007) | Mammography Screening | 1 to 5 "strongly agree to strongly disagree" | Not reported | Not reported | Used to tailor counseling |
| Pap Smear and mammography screening barriers (Glasgow et al., 2000) | Pap Smear Screening | 4-point "not at all to great deal" | Not reported | 3 factors identified with eigenvalues > 1.0 | Used to tailor counseling; women due for cancer screenings had greater barriers than those up to date |
| Barriers efficacy (Garcia & King et al., 1991) - Appendix 3 | Physical Activity | 0 to 100 Confidence | r = .67 | ∝ = .90 | Prospectively associated with exercise adherence |
| Barriers efficacy (Glasgow et al., 2001) | Multiple behaviors (for diabetes) | 1 to 5 "how difficult" and 0-10 "how confident can overcome" | Mean r = .60 (.43 - .80) | Mean ∝ = .90(.74 - .98) | Prospectively related to dietary, exercise, and stress management |
| Medication taking (Hong et al., 2006) | Medication taking | Definitely false (1) to definitely true (4) | Not reported | ∝ = .73 | Predicted HTN medication adherence in cross-sectional analyses |
| Barriers to CRC screening (Zheng et al., 2006) - Appendix 4 | Colorectal screening | 1-5 "strongly disagree to strongly" agree | Not reported | Not reported | Related to intention to follow-up abnormal FOBT result |
Measures of Cancer-related Barriers
Appendices 1-4 present examples of some of the most widely used types of barrier scales for health behaviors related to cancer prevention and management. The footnote to each table contains contact information to secure information about administration, scoring, norms, and interpretation. Appendix 1 asks smokers to rate their confidence that they can resist a variety of barriers (or temptations based on TTM theory). Appendix 2 is a mammography screening barriers scale to identify targets for intervention; the scale was used successfully to tailor counseling (Champion et al., 2007). Appendix 3 is an example of barriers efficacy related to physical activity (Garcia & King et al., 1991). Finally, Appendix 4 illustrates a 5-point "strongly agree" to "strongly disagree" response scale for barriers to colorectal screening (Zheng et al., 2006).
6. Summary
The concept of perceived barriers is both important and central to a variety of prominent health behavior theories. There are a number of validated barrier measures available for use that target screening for cancer and other diseases, and especially for preventive health behaviors. Additional research is needed to address issues such as: 1) the impact of culture, race, ethnicity, health literacy, and other factors on perceptions of barriers; 2) if a standard, feasible core set of barrier questions and responses can be identified by content area for the different purposes of prediction and individual tailoring of intervention; and 3) interpretive problems and lack of conceptual clarity that are discussed above (Glasgow et al., 2001; McCauley et al., 1998). Future research should also pay increased attention to emotional and "distress"-related issues that are proving to be of critical importance in chronic illness (Anderson et al., 2007; Fisher et al., 2007). A final topic for further research is the issue of barriers among patients who have several comorbid conditions and receive multiple health behavior recommendations. Such "high-risk" patients may face barriers that are qualitatively and quantitatively different than those experienced by those with fewer conditions (Bayliss et al., 2003).
As in many areas of research, several investigative teams have made progress, but often appear to be unaware of or not influenced by alternative approaches or developments in different areas. With barriers, the key issue is not the exact measure or analysis used, but how the results are interpreted. As with many attempts to apply theory to real-world health behaviors, there are challenges to appropriate operationalization and interpretation of results (Weinstein, 2007). Future research will likely see continued and expanded use of barrier concepts and measures, especially in areas such as barriers to genetic screening.
7. References
Anderson, D., Horton, C., O’Toole, M. L., Brownson, C. A., Fazzone, P., & Fisher, E. B. (2007). Integrating Depression Care With Diabetes Care in Real-World Settings: Lessons From Robert Wood Johnson Foundation Diabetes Initiative. Diabetes Spectrum, 20, 10-16.
Bandura, A. (1997). Self-efficacy: The exercise of control. New York: W.H. Freeman.
Bayliss, E. A., Steiner, J. F., Fernald, D. H., Crane, L. A., & Main, D. S. (2003). Descriptions of barriers to self-care by persons with comorbid chronic conditions. Annals of Family Medicine, 1, 15-21.
Becker, M. H., Maiman, L. A., Kirscht, J. P., Haefner, D. P., Drachman, R. H., & Taylor, D. W. (1979). Patient perceptions and compliance: Recent studies of the Health Belief Model. In R.B.Haynes & D. L. Sckett (Eds.), Compliance in health care (Baltimore: Johns Hopkins University Press).
Champion, V., Skinner, C. S., Hui, S., Monahan, P., Juliar, B., Daggy, J. et al. (2007). The effect of telephone versus print tailoring for mammography adherence. Patient Education and Counseling, 65, 416-423.
Chao, J., Nau, D. P., Aikens, J. E., & Taylor, S. D. (2005). The mediating role of health beliefs in the relationship between depressive symptoms and medical adherence in persons with diabetes. Research in Social & Administrative Pharmacy, 1, 508-525.
D'Zurilla, T. J. (1996). Problem-solving therapy: A social competence approach to clinical intervention. New York: Springer.
Fisher, L., Skaff, M. M., Mulllan, J. T., Arean, P., Mohr, D., Masharani, U. et al. (2007). Clinical depression versus distress among patients with type 2 diabetes: Not just a question of semantics. Diabetes Care, 30, 542-548.
Garcia, W. A. & King, A. C. (1991). Predicting Long-Term Adherence to Aerobic Exercise: A Comparison of Two Models. Journal of Sport & Exercise Psychology, 13, 394-410.
Glanz, K., Lewis, F. M., & Rimer, B. K. (2002). Health behavior and health education: Theory, research and practice. (3rd ed.) San Francisco: John Wiley & Sons.
Glasgow, R. E., Emont, S., & Miller, D. S. (2006). Assessing the delivery of the 5 "As" for patient-centered counseling: alternatives and future directions. Health Promotion International, 21, 2245-255.
Glasgow, R. E., Fisher, L., Skaff, M., Mullan, J., & Toobert, D. J. (2007). Problem-solving and diabetes self-management: Investigation in a large, multi-racial sample. Diabetes Care, 30, 33-37.
Glasgow, R. E., Gillette, C., & Toobert, D. (2001). Psychosocial barriers to diabetes self-management and quality of life. Diabetes Spectrum, 14, 33-41.
Glasgow, R. E., Toobert, D. J., Barrera, M., Jr., & Strycker, L. A. (2005). The Chronic Illness Resources Survey: Cross-validation and sensitivity to intervention. Health Education Research, 20, 402-409.
Glasgow, R. E., Whitlock, E. P., Valanis, B. G., & Vogt, T. M. (2000). Barriers to mammography and Pap smear screening among women who recently had neither, one or both types of screening. Annals of Behavioral Medicine, 22, 223-228.
Hampson, S. E. (1996). Illness representations and self-management of diabetes. In J.Weinman & K. Petrie (Eds.), Perceptions of illness and treatment: Current psychological research and applications (Chur, Switzerland: Harwood Academic).
Hill-Briggs, F. (2003). Problem solving in diabetes self-management: A model of chronic illness self-management behavior. Annals of Behavioral Medicine, 25, 182-193.
Hong, T. B., Oddone, E. Z., Dudley, T. K., & Bosworth, H. B. (2006). Medication barriers and anti-hypertensive medication adherence: The moderating role of locus of control. Psychology, Health & Medicine, 11, 20-28.
Leventhal, H. & Diefenbach, M. (1991). The active side of illness cognition. In J.A.Skelton & R. T. Croyle (Eds.), Mental representation in health and illness (pp. 246-272). New York: Springer-Verlag.
Locke, E. A. & Latham, G. P. (2002). Building a practically useful theory of goal setting and task motivation. A 35-year odyssey. American Psychologist, 57, 705-717.
McCauley, E. & Mihalko, S. L. (1998). Measuring exercise-related self-efficacy. In J.L. Duda (Ed.), Advances in sport and exercise psychology measurement (Morgantown, WV: Fitness Information Technology).
Montano, D. E. & Kasprzyk, D. (2002). The theory of reasoned action and the theory of planned behavior. In K. Glanz, F. M. Lewis, & B. K. Rimer (Eds.), Health behavior and health education: Theory, research and practice (3rd ed., San Francisco: John Wiley & Sons).
Ruelaz, A. R., Diefenbach, P., Simon, B., Lanto, A., Arterburn, D., & Shekelle, P. G. (2007). Perceived barriers to weight management in primary care--perspectives of patients and providers. Journal of General Internal Medicine, 22, 522.
Stokols, D. (2000). Social ecology and behavioral medicine: Implications for training, practice, and policy. Behavioral Medicine, 26, 129-138.
Velicer, W. F., DiClemente, C. C., Rossi, J. S., & Prochaska, J. O. (1990). Relapse situations and self-efficacy. Addictive Behaviors, 15, 217-283.
Weinstein, N. D. (2007). Misleading test of health behavior theories. Annals of Behavioral Medicine, 33, 1-10.
Whitlock, E. P., Orleans, C. T., Pender, N., & Allan, J. (2002). Evaluating primary care behavioral counseling interventions: An evidence-based approach. American Journal of Preventive Medicine, 22, 267-284.
Williams, G. C. & Deci, E. L. (1998). The importance of supporting autonomy in medical education. Annals of Internal Medicine, 129, 303-308.
Zheng, Y.-F., Sait, T., Takahashi, M., Ishibashi, T., & Kai, I. (2006). Factors associated with intentions to adhere to colorectal cancer screening follow-up exams. BMC Public Health, 6, 272.
8. Appendix 1: Self-Efficacy/Temptation Scale – Long Form
INSTRUCTIONS: Listed below are situations that lead some people to smoke. We would like to know HOW TEMPTED you may be to smoke in each situation. Please answer the following questions using a 5-point scale with 1 = NOT AT ALL TEMPTED AND 5 = EXTREMELY TEMPTED
| How tempted are you to smoke… | Not at all tempted | hNot very tempted | Moderately tempted | Very tempted | Extremely tempted |
|---|---|---|---|---|---|
| 1. At a bar or cocktail lounge having a drink. | 1 | 2 | 3 | 4 | 5 |
| 2. When I am desiring a cigarette. | 1 | 2 | 3 | 4 | 5 |
| 3. When things are just not going the way I want and I am frustrated. | 1 | 2 | 3 | 4 | 5 |
| 4. With my spouse or close friend who is smoking. | 1 | 2 | 3 | 4 | 5 |
| 5. When there are arguments and conflicts with my family. | 1 | 2 | 3 | 4 | 5 |
| 6. When I am happy and celebrating. | 1 | 2 | 3 | 4 | 5 |
| 7. When I am very angry about something or someone. | 1 | 2 | 3 | 4 | 5 |
| 8. When I would experience an emotional crisis, such as an accident or death in the family. | 1 | 2 | 3 | 4 | 5 |
| 9. When I see someone smoking and enjoying it. | 1 | 2 | 3 | 4 | 5 |
| 10. Over coffee while talking and relaxing. | 1 | 2 | 3 | 4 | 5 |
| 11. When I realize that quitting smoking is an extremely difficult task for me. | 1 | 2 | 3 | 4 | 5 |
| 12. When I am craving a cigarette. | 1 | 2 | 3 | 4 | 5 |
| 13. When I first get up in the morning. | 1 | 2 | 3 | 4 | 5 |
| 14. When I feel I need a lift. | 1 | 2 | 3 | 4 | 5 |
| 15. When I begin to let down on my concern about my health and am less physically active. | 1 | 2 | 3 | 4 | 5 |
| 16. With friends at a party. | 1 | 2 | 3 | 4 | 5 |
| 17. When I wake up in the morning and face a tough day. | 1 | 2 | 3 | 4 | 5 |
| 18. When I am extremely depressed. | 1 | 2 | 3 | 4 | 5 |
| 19. When I am extremely anxious and stressed. | 1 | 2 | 3 | 4 | 5 |
| 20. When I realize I haven't smoked for a while. | 1 | 2 | 3 | 4 | 5 |
SCORING INSTRUCTIONS: The Self-Efficacy/Temptation Scale (Long Form) provides a measure of confidence in resisting smoking in situations represented by the items. An overall score is computed by averaging across the 20 items. In addition, there are three subscales that measure broad aspects of self-efficacy to resist smoking: Positive Affect/Social Situations (items 1, 4, 6, 9, 10, and 16); Negative Affect Situations (items 3, 5, 7, 8, 18, and 19); Habit/Craving Situations (items 11, 13, 14, 15, and 20). Subscale scores are obtained by averaging the response to items within each subscale.
From "Relapse Situations and Self-Efficacy: An Integrative Model" by W.F. Velicer, C.C. DiClemente, J.S. Rossi, and J. O. Prochaska, 1990, Addictive Behaviors, 15:271-283. Reprinted by permission of Elsevier Science. (velicer@uri.edu)
9. Appendix 2: Mammography Screening Barriers
1. Compared with your other health problems, having a mammogram is not important
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
2. At your age, you do not need to have mammograms.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
3. You do not need a mammogram if you have a breast exam by a doctor.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
4. You are afraid to have a mammogram because it might show a problem.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
5. Having a mammogram is a lot of trouble for you.
(If a woman says, the mammogram is not too much trouble but going to the clinic or waiting is too much trouble, ask: Is what you have to go through to have a mammogram too much trouble?)
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
6. Having a mammogram is painful for you.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
7. Having a mammogram is embarrassing for you.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
8. You are worried about having a mammogram because you don't understand what will be done.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
9. You don't have the time to get a mammogram.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
10.Cost would keep you from having a mammogram.
(If woman asks how much a mammogram costs, say, "I'm not sure. It's different in different places. I just need to know if you think the cost of a mammogram would keep you from having one.")
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
11. Having a mammogram makes you worry about being exposed to the x-ray.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
12. You have trouble remembering to get a mammogram.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
13. People at the mammography centers are not friendly.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
14. A mammogram can help you find breast cancer when it is just getting started.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
15. Your doctor did not tell you that you should have a mammogram.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
16. Having a mammogram will decrease your chances of dying from breast cancer.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
17. Having a mammogram is the best way to find breast cancer when it is just getting started.
| Agree ---------- | strongly agree? Or | ____ (5) |
| agree? | ____ (4) | |
| Neutral/no opinion -------------------------- | ____ (3) | |
| Disagree ------ | disagree? Or | ____ (2) |
| strongly disagree? | ____ (1) | |
| Don’t know -------------------------------- | ____ (0) | |
10. Appendix 3: Barrier-based Exercise Self-Efficacy
Confidence Scale
| 0 percent | 10 percent | 20 percent | 30 percent | 40 percent | 50 percent | 60 percent | 70 percent | 80 percent | 90 percent | 100 percent |
| Not at all Confident | Somewhat Confident | Absolutely Confident | ||||||||
Confidence Rating
| Over the next six months I could exercise... | (0-100 percent ) |
|---|---|
| 1. When tired........ | _____________________ |
| 2. During or following a personal crisis........ | _____________________ |
| 3. When feeling depressed........ | _____________________ |
| 4. When feeling anxious........ | _____________________ |
| 5. During bad weather........ | _____________________ |
| 6. When slightly sore from the last time I exercised........ | _____________________ |
| 7. When on vacation........ | _____________________ |
| 8. When there are competing interests (like my favorite TV show)........ | _____________________ |
| 9. When I have a lot of work to do........ | _____________________ |
| 10. When I haven't reached my exercise goals........ | _____________________ |
| 11. When I don't receive support from family or friends........ | _____________________ |
| 12. Following complete recovery from an illness which has caused me to stop exercising for a week or longer........ | _____________________ |
| 13. When I have no one to exercise with........ | _____________________ |
| 14. When my schedule is hectic........ | _____________________ |
Garcia AW, King AC. Predicting Long-Term Adherence to Aerobic Exercise: A Comparison of Two Models. Journal of Sport & Exercise Psychology 1991;13:394-410. (abby.king@stanford.edu)
11. Appendix 4: Barriers to Colorectal Screening
| Perceived Barriers | Range or Category | Respondents mean (SD) |
|---|---|---|
| Misperception regarding the necessity of follow-up | ||
| CDE* are not necessary unless symptomatic | 1-5 | 1.8 (1.2) |
| CDE are not necessary for my age | 1-5 | 1.7 (1.1) |
| Discomfort with the CDE procedure | ||
| Having CDE would be embarrassing | 1-5 | 2.8 (1.5) |
| Bowel preparation for the CDE is too difficult | 1-5 | 3.8 (1.3) |
| Having CDE would be uncomfortable | 1-5 | 3.6 (1.4) |
| Having CDE would be painful | 1-5 | 3.6 (1.4) |
| Psychological costs | ||
| I will feel uncomfortable talking about CRC** | 1-5 | 2.7 (1.4) |
| I am afraid of finding cancer | 1-5 | 3.5 (1.4) |
| Practical Barriers | ||
| I am too busy to undertake follow-up examinations | 1-5 | 1.8 (1.1) |
| I have other things to do that are more important than undertaking follow-up examinations | 1-5 | 1.4 (0.9) |
| Having CDE would cost too much money | 1-5 | 1.8 (1.1) |
* Complete Diagnostic Evaluations
** Colorectal Cancer
Zheng Y-F, Saito T, Takahashi M, Ishibashi T, Kai, I. Factors associated with intentions to adhere to colorectal cancer screening follow-up exams. BMC Public Health 6:272 (teiyf-tky@umin.ac.jp)
References
Velicer, W. F., DiClemente, C. C., Rossi, J. S., & Prochaska, J. O. (1990). Relapse situations and self-efficacy. Addictive Behaviors, 15, 217-283.
Champion, V., Skinner, C. S., Hui, S., Monahan, P., Juliar, B., Daggy, J. et al. (2007). The effect of telephone versus print tailoring for mammography adherence. Patient Education and Counseling, 65, 416-423.
Glasgow, R. E., Whitlock, E. P., Valanis, B. G., & Vogt, T. M. (2000). Barriers to mammography and Pap smear screening among women who recently had neither, one or both types of screening. Annals of Behavioral Medicine, 22, 223-228.
Garcia, W. A. & King, A. C. (1991). Predicting Long-Term Adherence to Aerobic Exercise: A Comparison of Two Models. Journal of Sport & Exercise Psychology, 13, 394-410.
Glasgow, R. E., Gillette, C., & Toobert, D. (2001). Psychosocial barriers to diabetes self-management and quality of life. Diabetes Spectrum, 14, 33-41.
Hong, T. B., Oddone, E. Z., Dudley, T. K., & Bosworth, H. B. (2006). Medication barriers and anti-hypertensive medication adherence: The moderating role of locus of control. Psychology, Health & Medicine, 11, 20-28.
Zheng, Y.-F., Sait, T., Takahashi, M., Ishibashi, T., & Kai, I. (2006). Factors associated with intentions to adhere to colorectal cancer screening follow-up exams. BMC Public Health, 6, 272.

